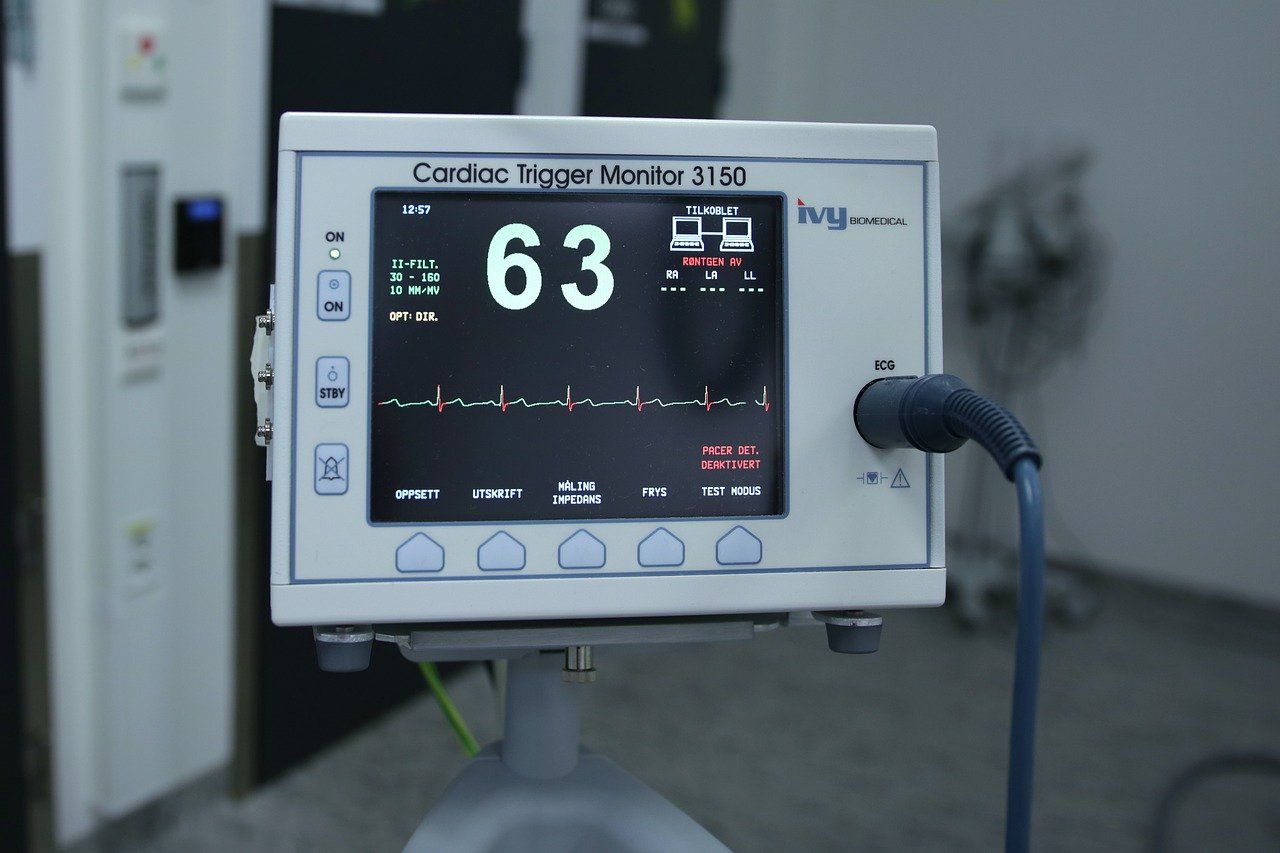
Much of the current debate about euthanasia takes place on a largely philosophical level. As we weigh the arguments, discussing all the pros and cons in the abstract, we can easily miss the real issues. What are they?
People
The debate is about people, not abstractions
. It is very easy to be taken up with the theories, philosophies, or even the ethical arguments. But in the last analysis we are discussing the end of life for individual people.
Our responsibility is to meet their real needs, not to justify an opinion or to support a position. Each person is different, and we need to get alongside the individual and respond to their specific life-situation with life-affirming responses. Death is no answer to any need.
The many
It is about the many, not the few. The number of cases for which the extreme measure of euthanasia can be argued is very small.
If it were ever introduced, even if restricted to difficult clinical situations, there would be a strong temptation to save resources by bringing life to an end sooner, rather than later. Many would be at risk from bad or self-interested decision-making.
The arguments about euthanasia often revolve round difficult cases, some of them very real and intensely problematical, some of them largely hypothetical. Any lawyer will tell you that ‘hard cases make bad law’.
The important issue is that laws based on extraordinary situations would affect a much broader spectrum of ordinary clinical practice. They could and would be applied to many situations which are currently, and appropriately, handled without recourse to the deliberate ending of a life.

Compassion
The debate is about compassion, as a standard, not as an exception.
Some time ago a paper appeared in the British Medical Journal (1) reporting a study of the care of dying patients in four West of Scotland hospitals.
With the full cognisance of medical and nursing staff, a non-participant observer (an experienced nursing tutor) monitored the clinical interaction between dying patients and the staff of the wards in which they were treated.
The abstract of the paper reads as follows: ‘More than half of all patients retained consciousness until shortly before death. Basic interventions to maintain patients’ comfort were often not provided.
‘Oral hygiene was often poor, thirst remained unquenched, and little assistance was given to encourage eating. Contact between nurses and the dying patients was minimal; distancing and isolation of patients by most medical and nursing staff were evident; this isolation increased as death approached.’
Not all of the observed practice was poor. Four of the fourteen consultants and seven of the twenty-two senior nurses were seen to have a greater number of encounters with dying patients than the average.
They spent time with the patient, used their name, established eye contact, took steps to meet their clinical and personal needs, and maintained contact with them until death.
The majority, however, concentrated on the disease process, the physical deterioration and the attempted relief of some of their symptoms. Personal contact was minimal or absent, and, as death came nearer, they distanced themselves from the patient.
The time spent at a patient’s bedside related directly to the continuation of active medical intervention. When this was scaled down and death became imminent, the time given significantly diminished.

Standards of care
The paper reminds us that compassion, in the sense of involvement by caring staff, is less common than we might think. But without the standard of compassion demonstrated in the better units, dare we risk introducing a ‘way out’ for busy staff who do not want to be compassionately involved?
We need to ask: Are our standards of care all they might be? Are they all we think they are? Are they all we claim them to be? Until they are, whether we like it or not, the advocates of euthanasia will press their case.
Caring
It is about how we care for everyone, not just the dying.
There is, in fact, little difference between the needs of a seriously ill person and one who is terminally ill. The best answer to complaints of poor care on the one hand, and demands for euthanasia on the other, is to set high standards of care.
These will require us to respond personally and compassionately to the individual, rather than apply a blanket solution to every similar situation. To kill cannot, ever, be a substitute for caring.
Part of the problem lies in modern society’s altered attitude to dying. There have been significant shifts when compared with former attitudes. Consider three such changes.
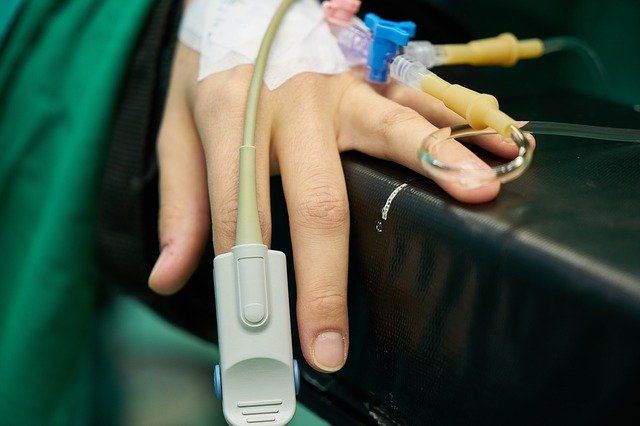
Non-acceptance
In the past, when medical intervention in critical illness was less likely to be effective, it was more widely accepted that death was inevitable. But as life-support and resuscitation measures have become more effective, this acceptance has been replaced by the expectation that ‘Medicine must do something about it’.
This opinion prevails whether the technology or resources are available or not. The extension of this idea may be: ‘If Medicine can’t do anything about it, let’s get it over quickly’.
Secularisation
As religious faith has been eroded by secular and materialistic philosophies, the view is expressed: ‘There is no life, and therefore no responsibility, after death’. The rejection of personal accountability for the outcome of life, and of a future beyond death, has led to a cheapening of life.
Death has been trivialised to the point that it is perceived as merely the end of existence for the individual: ‘If there is nothing after death there is no reason not to end life’.
Increase in anxiety
One might think that such an attitude would reduce anxiety regarding death. Yet the fear of death persists and has been supplemented by the fear of the process of dying.
This fear relates to the symptoms the person may suffer, that suffering may be unrelieved, and that the process of dying may be unduly prolonged.
Many people still fear death and its consequences because of a deep uncertainty about what may lie beyond. Such an anxiety can only be relieved by the assurances and positive hope of faith.
Without such faith one might argue: ‘If dying is the thing people fear, then it is better to reduce the length of the process’. Thus euthanasia is made to appear as the ultimate compassionate act, and the suicide of the terminally ill is given a rationale.
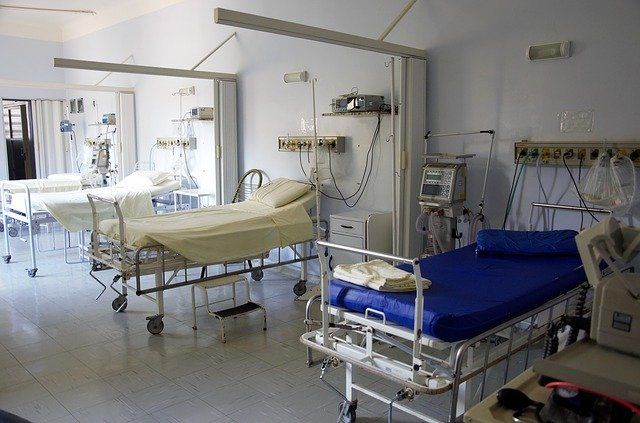
The risk of abuse
Our next concern must be the risk that power and clinical freedom would be abused. These things are inherent, of course, in all clinical relationships, and the overall risk of deliberate abuse is probably quite small.
There is, however, a much greater risk of careless abuse, or abuse by default. If the option to kill the patient were to be available to doctors it would be all too easy, especially under severe emotional duress, to ‘go along’ with the wishes of patients or well-meaning relatives.
The clinical relationship, by definition, is one of trust. The question must be asked whether it could remain so if the doctor has the power to bring life to an end.
The doctor’s traditional, historic and moral commitment is to life. Indeed, the doctor may be most helpful when asserting the value of life, when the patient or their relatives have lost sight of it. It would, therefore, be a major change to introduce death as a legitimate clinical option.
At present, however distressed, the patient does not expect his doctors to suggest death as an option. With legalisation of euthanasia, the fear that they might do so introduces further anxiety into the already tense situation of serious illness.
Change in the norm
To legalise life-termination, under whatever guise, would decrease the consideration given to other treatment options. It would also introduce the idea that euthanasia is the right, the normal, or even the obligatory means of bringing serious illness to an end.
The analogy with abortion-law reform is self-evident. The alternatives available to a woman faced with an unwanted pregnancy are seldom presented because the immediacy of termination is so attractive.
The negative consequences are ignored or played down, and the ‘easy’ way out is accepted as the norm. The woman who opts for any alternative is made to feel abnormal, and may be openly criticised for her decision.
Already there are elderly and disabled people who feel they are a burden to their relatives, and feel an obligation to remove that burden. It is a sad reflection on our reputedly compassionate society that this negative mind-set could be reinforced by the proposal that doctors should be free to remove the burden.
Wrong questions
How much better to reassert the intrinsic value of the patient by the affirmation of life! Looking to euthanasia as a primary means to relieve suffering implies losing hope when we most need help to find it.
It means concentrating on the loss of life instead of finding meaning in life. It turns the focus on self and suffering when we most need to look beyond them.
There is, then, a real risk that the debate may obscure these issues. We may begin to see withdrawal of treatment, or the assisting of suicide, as the only solution, when valid alternative measures are available. We may see death as the best answer, when asking all the wrong questions.
If we lose sight of the priority of caring for people, our society will become less, rather than more, compassionate.
Opposition not enough
However, mere opposition to euthanasia in the context of debate is not enough! We must also be active in establishing good, involved, personal care for the ill and disabled, whether terminally ill or not.
Hostel, hospice, community and other supportive care provisions need our support. There is a major need to train and educate doctors, nurses and healthcare workers (whether in general practice, hospital or nursing homes) to provide better supportive care for patients and for relatives.
(1) Mills M. et al, Care of Dying Patients in Hospital, BMJ 309 (1994) pp. 583-586.
An edited version of an article published by the Christian Institute in January 2000